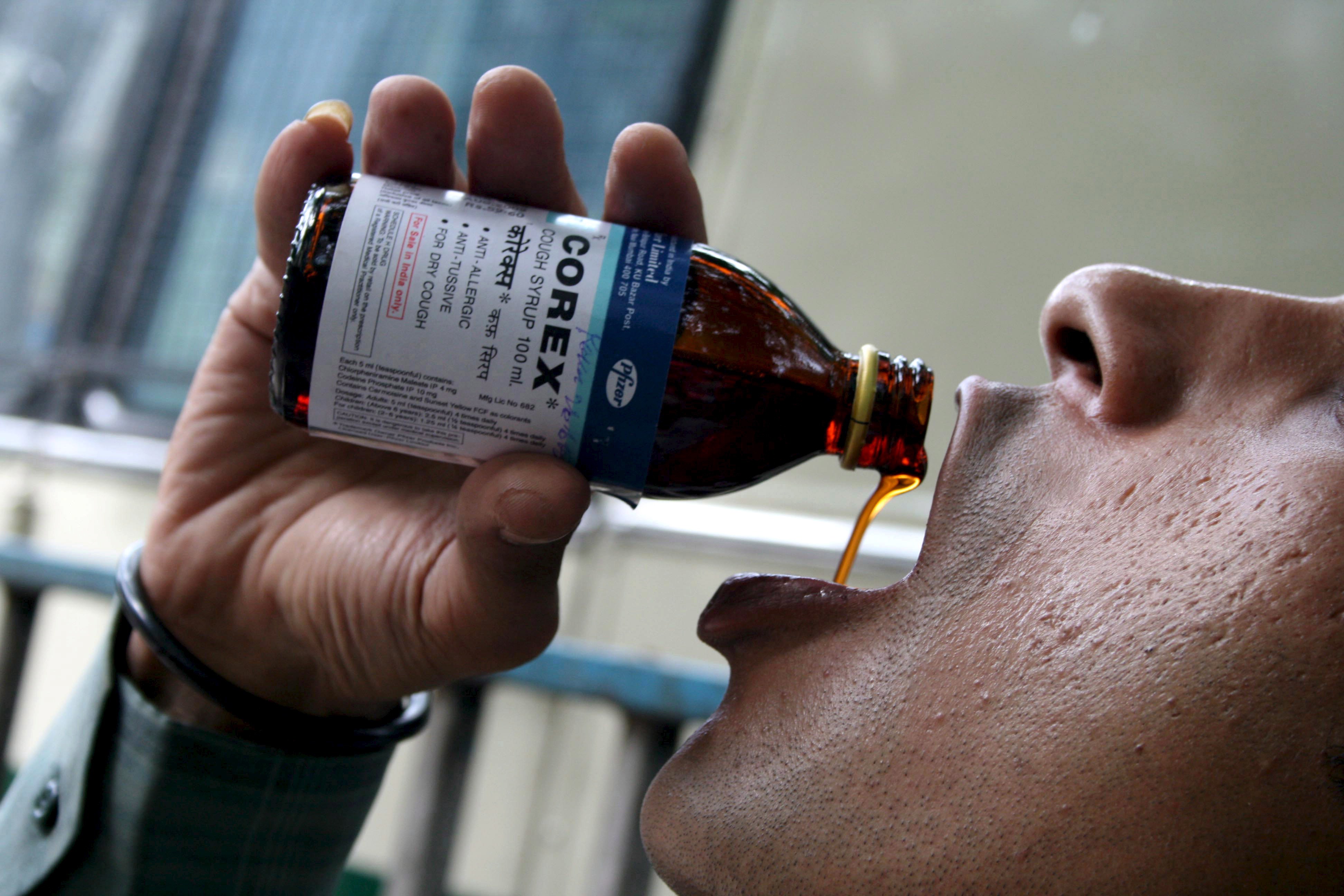
Misuse of opiates and prescription medication, in general, is a longstanding and continuing public health challenge in Nigeria. Codeine, an opioid substance often used in various preparations as an antitussive
(cough suppressant)3 and analgesic4 agent,and Tramadol5 , a synthetic opioid analgesic,usually prescribed for pain of moderate to severe intensity are creating drug-dependent users across a broad spectrum of cultures and social classes throughout the country.
Images of hijab-wearing teenagers apparently addicted to codeine and similar opioid substances have been extremely prominent on social media and in local and international news coverage in recent months.
A sense of local outrage demonstrated amongst citizens, and negative global publicity generated by this problem has prompted a series of highly emotive responses from a cross-section of civil society in addition to a number of policy capitulations from government-affiliated agencies6.
A seemingly inexorable rise in the number of young and married women addicted to opioid substances in the more socially conservative (northern) states of Nigeria, such as Kano and Jigawa, is substantiated mainly by anecdotal evidence and opinion pieces based on news media reports7.
As is the case in the study of other issues of public health significance in Nigeria’ health sector, an understanding of the scope and exact nature of the problem is hindered significantly by the absence of much-needed
empirical data to support articulation of a public health policy response. Despite suggestions of an emerging problem in vulnerable population groups with particular sociocultural patterns and lifestyles, the socially disruptive consequences of opiate addiction are most certainly not confined to communities residing in any particular region of the country. The consensus view, therefore, is of a complex and challenging health and social care problem,approaching epidemic proportions and worthy of a strategic national response.
Epidemiological origins
In reality, Nigeria has over the past three decades, endured the challenges of one form of drug addiction problem or another. In a 1991 review of the clinical implications of drug abuse in Nigeria, Abiodun (1991), established the longstanding nature of the problem as follows – ‘drug abuse has become a major public health problem in Nigeria. Alcohol, cannabis,psychostimulants and hypnosedatives are the most commonly abused drugs. Drug abuse in the country now starts at an early age and cuts across all age groups8.’
In May 2018, the Director-General of the National Agency for Food and Drug Administration and Control (NAFDAC) issued a statement suggesting the reason for the current codeine crisis to be ‘…inadequate NAFDAC presence at various ports of entry, leading to significant levels of smuggling and importation of considerable amounts of products with potential for abuse and unregulated distribution.’
The statement goes further to identify a lack of multidisciplinary stakeholder collaboration and inadequate monitoring of open markets by agencies such as the Pharmacists Council of Nigeria (PCN), NAFDAC and the Federal
Ministry of Health (FMoH) as further reasons for enforcement failures leading to the current situation.
However, the most cursory reflection on the facts of the matter highlight two critical issues of importance to the construction of any informed critical appraisal of the subject under discussion – Why, in the first place, is there a high demand for unlicensed use of opiaterelated medicines? More to the point – Is there an epidemiological reason for the high use of Codeine and Tramadol in particular demographics and society in general?
In attempting to resolve the problem of opiate misuse in present-day Nigerian society,therefore, there is a crucial need to articulate a clear understanding of the spectrum of sociocultural triggers potentially responsible for the dilemma that confronts its citizens. The next few paragraphs will attempt a broad categorisation of these triggers in general terms.
Inequality & sociodemographic predispositions
Nigeria has an estimated population of 180 million people comprising more than 250 ethnic groups speaking (approximately) 500 languages and dialects. 50% of the population are urban dwellers, about 50% are Muslim,
40% Christian and 10% Animist. Most of the community is young with roughly 42.5% under the age of 14 years9.
Nigeria is also a country of extreme paradoxes. Despite having a GDP of over US$400 billion, the country’s Human
Development Index (HDI) in 2016 was 0.527 (ranked 152 out of 188 UN members states10). As Oxfam have taken great care to point out in the past, ‘Nigeria is not a poor country, yet millions are living in hunger’. The charity
estimates the combined wealth of the five wealthiest men in Nigeria at £29.9billion, a sum capable of ending the extreme poverty of its people on a national scale11.
Between 1960 and 2005, approximately US$20 trillion was unlawfully appropriated by public office holders representing several governing regimes. In 2012, Nigeria spent 6.5% of her national budget on education and
3.5% on health. By comparison, Ghana spent 18.5% and 12.5% respectively on these sectors.
These statistics underscore an essential and incontrovertible principle that countries with high levels of inequality perform poorly in the development stakes. Pickett and Wilkinson in their 2009 book titled ‘the spirit level: why more equal societies almost always do better’,describe ‘the pernicious effects’ of inequality on society and recognise substance misuse as one of 11 health and social-related problems worsened by the current dynamics of unequal wealthy societies12.
Sociocultural dimensions of substance misuse & poor mental health
The sociocultural factors underlying individual and societal predispositions towards substance misuse may be considered in terms of 3 important themes – Entitlement, Embitterment and Estrangement.
These ‘3 E’s’ are indeed simplifications of complex socio-cultural phenomena which although unlikely to survive robust critical scrutiny, offer considerable insight into the psychological and social underpinnings of drug
misuse in present-day Nigerian society. Also,they provide a basis upon which to begin an exploration of cause, correlation, associations and effects of this clear and present danger to societal cohesiveness and psychosocial
wellbeing.
1. Entitlement
Civil society in Nigeria, with its not insignificant layer of wealthy individuals and families,demonstrates a distinctly plutocratic inclination towards ostentatious displays of wealth,patronage and influence. The self-indulgent excesses of many of the rich and famous have tended to involve a liberal attitude towards drug-taking and associated forms of illicit and anti-social behaviour.
The sense of impunity and feeling of entitlement often demonstrated by this influential class of society, combined with the twin problem of experimental curiosity and peer group pressure influence experienced especially among the youth, may contribute significantly to the misuse of all classes of drugs, including opioids, in the general population13.
2. Embitterment
One incontestable feature of an unequal plutocratic society is the feeling amongst the majority of its citizens, of being left behind. The daily struggle for ‘survival’ is ironically not a problem confined strictly to the lower segments of society but is also the lived reality of the professional classes.
The sheer stress of living conditions in such an environment brings about a profound feeling of embitterment, based on a sense that society is inherently unfair and that material resources are limited to those who by patronage or mutual self-interest have existing relationships with those in power. Such embitterment is
often manifest in individuals by way of poor mental and physical health, and there is considerable evidence in support of a strong bi-directional relationship between depression and substance misuse.
A culture of early marriage, early parenthood and resentment of restrictive cultural norms imposed on women in some communities and families may also contribute towards a state of depression and subsequent drug addiction. Such women, despite these restrictions, are often introduced (usually through electronic and social media) to alternative cultures and lifestyles, which may include drug-taking activity and other similar practices.
3. Estrangement
At the bottom of the pile in an unequal society,are young people and families consigned to perpetual penury by societal strictures. Lorant et al. (2003) assert that low socioeconomic status is generally associated with high
psychiatric morbidity and inadequate access to healthcare.
The reality of less sophisticated coping mechanisms, destabilising life events, undue stress exposure and weaker social support systems are some of the risks disproportionately borne by the poor in society.
It is therefore conceivable, in at least a minority of cases, that in seeking to alleviate the burden of poverty imposed by these unfair and opportunity-denying societal arrangements, a career in criminality is seen as the most viable way out.
The use of illicit substances to reduce anxiety, obviate the fear of capture or to lessen the burden of guilt having committed a series of violent misdemeanours is almost always inevitable. The correlation between the criminal underworld, drug dealing and substance misuse is well established and offers an additional path to the problem of opioid drug dependency.
Responding to ‘wicked’ dynamics
A ‘wicked’ problem, often a social or cultural problem, is a problem generally regarded by society as complex, intractable, open-ended and unpredictable. A range of challenging issues such as global warming, drug abuse,
nuclear weapons and natural disasters may fall into this category. Rittel & Webber (1973) specified ten characteristics of wicked problems in relation to social policy14.
Four applications of this principle are of particular relevance in unravelling the ‘wicked’ nature of prescription drug abuse in Nigeria.
1. Incomplete and contradictory knowledge about the full extent of opioid drug use and dependence in Nigeria.
2. A wide variety of people with very different but strongly held opinionsabout the nature of the problem – A prominent northern leader was quoted as blaming Ibo traders with local Hausa accomplices for the codeine problem in Kano.
1. NAFDAC to suspend issuance of import permits for codeine and tramadol
2. Recall of all cough preparations in circulation
3. Manufacturers to account for the disposal of codeine-containing preparations and tramadol
4. Deadline for manufacturers to replace codeine-containing cough syrups with appropriate substitutes
5. Audit of all codeine-containing cough syrups in the country
6. Reactivation of prescription policy
7. Strengthening of the Pharmacists Council of Nigeria (PCN)
8. Ministry of Health to collaborate with regulatory agencies to strengthen existing legal instruments
9. PCN to develop information, Education and communication materials on drug abuse
10. Ministry of Health to partner National Orientation Agency (NOA), Nigeria Football Federation (NFF), Actors Guild of Nigeria, Performing Musicians of Nigeria and other celebrities to drive national campaign against drug abuse
11. Ministry of Health to ensure drug treatment intervention for substance abusers across the spectrum of healthcare delivery
12. Civil society organisations to be supported to deliver effective sensitisation, prevention,treatment and rehabilitation services on behalf of the population
13. Ministry of health to continue advocacy through the legislative arm of national government, state governors, religious leaders and traditional leaders
Table 2: 13 CCRWG Recommendations, 1st May 2018
3. There is an as-yet uncalculated financial burden to be borne in addressing the complex issues raised by NAFDAC at the same time as raising public health awareness (as recommended by the CCRWG) and providing adequate infrastructural and human capital resources for rehabilitating dependent opioid users.
4. The opioid addiction crisis is part of a matrix of interconnected social, cultural and economic problems that assail the body politic and civil society in Nigeria.
In a memorandum submitted on the 1st of May 2018, the Codeine Control and other Related Matters Working Group (CCRWG)outlined 13 recommendations (summarised in table 2) designed to ’halt the menace of codeine, tramadol and other related substances of abuse.’
The next few paragraphs consider the immediate actions recommended by the CCRWG and attempt to evaluate the likely impact of these recommendations in light of the ‘wicked’ nature of the problem they propose to resolve.
One of the first observations to note,in considering the detailed set of recommendations submitted by the CCRWG
is the absence of an appropriate measure of success to indicate at some suitable stage that ‘problem’ has been resolved.
Additionally, owing to the multi-faceted nature of the problem that exists, it is likely to prove challenging to conclude in the present circumstances that measure 1 (import restrictions) would necessarily deal with the
problem or that measure 2 (product recall) is potentially enforceable in the current environment.
The appeal for collaborative joint working between various government agencies,regulatory bodies and elements of civil society appears not to appreciate in full, the divergent (inter-agency) interests at play in undertaking
such endeavours.
‘Globalising’ our approach
It is of course, much easier to critique potential solutions already proffered, that to generate ffective alternatives anew. However, given the complicated nature of the problem under review, it is essential to resist the ever-present temptation to find a ‘one-stop’ solution to the public health challenges of this social health
dilemma. It must indeed be said that a single comprehensive human response is almost never possible.
Nevertheless, the working recommendations offered by the CCRWG are an important staging post in a longer journey
towards coming to grips with the sociological and public health challenges presented by drug misuse. They represent a necessary opportunity to reflect on the origins and effects of the opiate abuse crisis in Nigeria and to formulate a coherent and rigorous strategic response designed to address the problem at hand.
On the 5th of February 2018, the Nigerian government launched 4 opiaterelated policy documents.
- National Policy for Controlled Medicines
- National Guidelines for Quantification of Narcotic Medicines
- National Guidelines for the Estimation of Psychotropic Substances and Precursors
- National Minimum Standards of Drug Dependence
Table 3: Codeine-related policy documents, FMoH, 5th Feb 2018
Nigeria would most certainly benefit from the adoption of a more global approach to the resolution of modern problems as well as glean further understanding from the policy responses of other nations with contemporary
experiences of a similar nature. It may be useful for example, to consider how the federal and state governments in the United States are dealing with their Oxycontin abuse epidemic or perhaps to understand how the Dutch and the
Portuguese governments have so far confronted the problem of drug abuse in their own environments.
Far from attempting to suggest that these countries have evolved the perfect sociological and policy solutions and that all we need do is ‘copy’ their ‘tried and tested’ initiatives, this is no more than an exhortation to expose ourselves to the accumulated wealth of global knowledge on the subject, and to adapt transferable learning in dealing with our own problems.
Having said this, the government’s implementation of the ‘National Drug Control Master Plan of Nigeria (2015-19)15 in response to the EU-funded collaborative project titled,‘Response to Drugs and Related Organised Crime in Nigeria (2013 – 2017)16’ is a significant step in the right direction. 4 hugely important policy documents (table 3) published subsequently (on the 5th of February 2018) reflect a culmination of the work so far conducted in this area and the fruit of broader collaboration in attempting to resolve the local effects of a more global and wide-ranging phenomenon affecting the lives of people of all ages, cultures, nationality and socioeconomic
backgrounds17.
In conclusion
The epidemiological origins of the substance misuse problem in Nigeria are in very many ways, unique. The peculiarities of Nigeria’s socioeconomic, cultural and public health landscape in addition to the overall
construction of the nation’s civil society are pointers to the need to formulate our own robust and fit-for-purpose responses to the questions raised by this extremely troubling issue.
There is an urgent need to deal comprehensively with the wider governance issues presented by the administration of prescription medication in general and more specifically with the regulation of unintended uses of opiate medication and support for individuals affected by substance misuse. Clarifying the way in which frame the problem
and therefore go about finding solutions is an important part of this process.
It is not unreasonable to suggest that if the policy solutions so far proposed do not, within a reasonable timeframe, succeed in bringing about the desired level of correction to this extremely challenging and complicated
problem, there exists a realistic prospect of significant socioeconomic and public mental health upheaval in the years to come. This article is intended as a small contribution to our understanding of the intricacies of the journey ahead.

Disclosure forms provided by the author are available at NEJM.org.
Editor’s note:
Author Affiliations
Supplementary Material
| Disclosure Forms | 83KB |
Add your Comment
Add your Comment
Leave a Reply
You must be logged in to post a comment.
BHQJ 2018 ; 001:34-36
Related Article 
Medical Negligence & the Law5th May 2018 . Atrogenic harm is a matter of significant concern in Nigeria admin
Colorectal Cancer Overview5th May 2018 . [dkpdf-columns columns="3" equal-columns="false" gap="10"] Introduction Colorectal cancer is a major admin
Funding Healthcare Services in Nigeria – A conundrum of demand, policy and supply!5th May 2018 . [dkpdf-columns columns="3" equal-columns="false" gap="10"] Doctor, I happy say na you admin
5 “Provocations” of Healthcare Quality Reform6th May 2018 . [dkpdf-columns columns="3" equal-columns="false" gap="10"] n the four decades since he admin
Health Insurance, Activism & Urgent Change6th May 2018 . [dkpdf-columns columns="3" equal-columns="false" gap="10"] AR: Dr Soyinka, it’s wonderful to admin
Anne Olowu talks about her “Masterclass” experience6th May 2018 . [dkpdf-columns columns="3" equal-columns="false" gap="10"] As I suspect is the case admin
Stomach & Oesophageal Cancer in Nigeria6th May 2018 . [dkpdf-columns columns="3" equal-columns="false" gap="10"] Gastric and Oesophageal (Upper GI) cancers admin
Setting out the Stall!7th May 2018 . [dkpdf-columns columns="3" equal-columns="false" gap="10"] "The drawbacks of our false knowledge admin



Leave a Reply
You must be logged in to post a comment.